Dentists, doctors and medical researchers have known for years that a link exists between diabetes and periodontitis, or gum disease, but they’ve struggled with pinpointing the exact origin of the connection. New research indicates that the connection has to do with changes in the oral microbiome (the collection of bacteria and other microbes that live in our mouths) of diabetes patients once blood sugar rises and hyperglycemia develops.
How Does Gum Disease Develop?
Diabetes weakens the body’s immune system, so patients are already more susceptible to infection, said Dr. John Pappas, DDS, of Arcadia Dental Arts in Phoenix, Arizona.
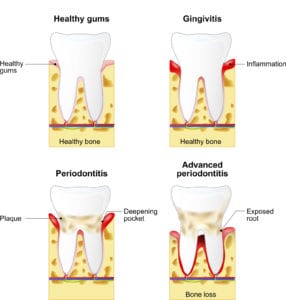
“Poor oral hygiene can lead to a buildup of bacteria and plaque on and around teeth,” he said. “The first stage of gum disease, called gingivitis, becomes evident with bleeding, swollen and red gums in many cases.”
According to Pappas, this first stage of gum disease is reversible with proper care. However, if left untreated, it can develop into the more serious stage of gum disease, called periodontitis. At this stage, the gums begin pulling away from the teeth where the pockets of infection have begun to form. Over time, it can lead to loss of bone and teeth.
Shift in Oral Microbiome Evident
The new study, conducted by researchers from the University of Pennsylvania, was published in the journal Cell Host & Microbe. Findings showed that changes in the oral microbiome of patients with diabetes caused a shift in the microbiome’s pathogenicity. Pathogenicity is the potential ability of an organism to cause disease. In patients with diabetes, these shifts in the oral microbiome show an increase in its pathogenicity, which could explain the susceptibility to gum disease.
The changes in the oral microbiome were also associated with inflammation and bone loss, both symptoms of periodontitis. The researchers studied mice with diabetes and discovered that diabetic mice actually had the same or similar oral microbiome as their healthy colleagues until they developed high blood sugar and became hyperglycemic. At this point, their oral microbiomes changed and the diabetic, hyperglycemic mice showed a less diverse community of bacteria in their microbiomes.
To further test their results, the scientists transferred microorganisms from the diabetic mice to the healthy mice and discovered that by simply transferring the oral microbiome of the diabetic mice, the healthy mice had 42 percent less bone.
Oral Care Recommendations for Diabetes Patients
Since controlling blood sugar levels can help control the risk for gum disease, Pappas recommends patients with diabetes remain vigilant about blood sugar and treatment with a doctor. Once infection occurs, healing can be prolonged due to the nature of diabetes.
“The biggest cause of gum disease is lack of oral hygiene, so maintaining a vigilant and effective oral care routine is key. Flossing gently and brushing teeth twice a day with a soft-bristled brush is the best thing you can do to help prevent gum disease,” Pappas said. In addition, Pappas recommends patients with diabetes see their dentist at least every six months to spot any problem areas early.